For as long as I can remember, being described as “yellow” and getting tired quickly have always been a part of my life. At first, it seemed normal — after all, kids get tired after playing, they tease each other, right? But as I grew older, it became clear that what I was experiencing wasn’t just ordinary tiredness. Simple activities like climbing a flight of stairs or spending a day at school left me completely drained. I could not even spend 30 mins playing basketball or running track with the same students in my class.
After years of uncertainty, I was finally diagnosed with Congenital Dyserythropoietic Anemia Type 2 (“CDA Type 2”), a rare genetic blood disorder.
The Diagnosis: An Answer, but Not a Solution
I was fairly young when I was diagnosed with CDA Type 2. Being told I had CDA Type 2 was a mix of confusion and fear. On one hand, I finally had an explanation for why I felt the way I did, although I did not truly understand it. On the other hand, my parents realized I had a condition that would require lifelong management.
CDA Type-2 affects how my red blood cells are produced and function. Instead of normal, healthy cells, my body produces cells that are malformed and don’t work as they should. This leads to chronic anemia, meaning my blood can’t carry oxygen as efficiently.
When I was diagnosed, my doctor explained that the condition is caused by a mutation in the SEC23B gene — a tiny error in my genetic code that has a big impact on my life. Hearing the word “rare” attached to my condition was both interesting and overwhelming. Few people had even heard of CDA, let alone Type 2, which made me feel like I was very special as a child, although rapidly understanding that it is more curse than privilege.
Growing up with CDA Type-2
Rizk Hospital’s special star
To those familiar with chronic illnesses, frequent doctor visits, checkups and hospital admissions are a standard thing. How does it apply to someone like me? Well it means having regular CBC Tests every month (CBC = Complete Blood Count), constantly visiting Hematologists and having to visit the hospital so frequently that you start to become famous with the nurses. (And we’re not talking George Cloony famous).
Why do I visited the hospital so frequently you ask? Well the first symptom of CDA Type-2, if you’ve been paying attention to the lesson above, is the anemia and extremely low blood count. This translates to little old me having to go to the hospital every 3 to 4 months, have 2 units of O+ blood transfused into my body, and then sent home to continue living my life semi-normally.
Ironically yes, my blood type is O+, which is supposed to be a universal donor 🤣
Eventually, I became famous in LAUMCRH (previously Rizk Hospital), and the nurses started to remember me as I visited more and more, and the transfusions got easier to digest every time, but both myself and my parents.
Time going by
As the years go by, the medical hope shifts to puberty. My main doctor tells my parents:
Ah! When he reaches 18, there is a chance he will need less transfusions.
As the months passed by, taking my teen years with them, that statement held true. My blood count started to reduce less over time (still being constantly low), my transfusions were less frequent (increasing to 5–6 months in frequency) and my fatigue was less prominent (I could at least play ping pong now!).
Living with the Symptoms
I would say the most challenging part of living with CDA Type 2 is the constant fatigue. It’s not the kind of tiredness you can fix with a nap or a good night’s sleep; it’s an ever-present weight. My energy levels fluctuate, but they’re never as high as I’d like. As I grew older, most of my days now I can push through and live almost normally, but there are also days when getting out of bed feels like running a marathon, and the blood count plunges back into the abyss.
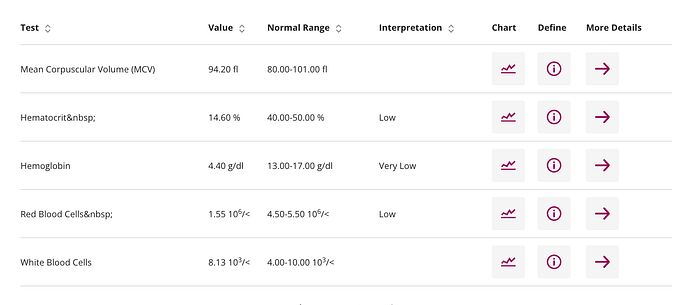
In addition to fatigue, I deal with jaundice, which gives my skin and eyes a yellowish tint due to excess bilirubin. It’s a visible reminder of my condition, and sometimes it’s hard to explain to people why I look the way I do. Splenomegaly — an enlarged spleen — is another challenge. My spleen works overtime to filter out the abnormal red blood cells, and as a result, it’s bigger than it should be. This can cause discomfort and increases the risk of complications.
As it stands today, I have a spleen of 22 CM in diameter. Ask your doctor and see his reaction, it’ll be fun. The cherry on top of all that is the constantly low count of red blood cells in my blood stream. Since they are malformed, and the spleen constantly destroys them, the Hemoglobin Count (Red Blood Cell Count) in my blood stream is always 50% below the norm (on a good day).
Managing the Condition
There’s no cure for CDA Type 2, so my treatment focuses on managing symptoms and preventing complications. Regular blood tests are a routine part of my life to monitor my hemoglobin levels and check for iron overload, a common issue in people with CDA. Since my body absorbs too much iron, I need to be vigilant about iron chelation therapy to prevent damage to my organs.
Blood transfusions are something I’ve had to face during particularly severe episodes of anemia. While they help temporarily, they can worsen iron overload, so they’re not a perfect solution. Doctors have mentioned bone marrow transplantation as a potential cure, but it’s a major procedure with significant risks, so for now, it’s not on the table.
Staying Hopeful
Living with CDA Type 2 is a constant balancing act. I have to listen to my body and prioritize my health, even when I’d rather ignore it and pretend I’m fine. While the physical symptoms can be overwhelming, I try to focus on what I can do rather than what I can’t.
There’s also hope in the advancements of medical research. Gene therapy and improved treatments are on the horizon, and I dream of a day when conditions like CDA Type-2 can be permanently cured without the risks of current options. Until then, I’ll continue to navigate this journey one step at a time, grateful for the support of my family, friends, and the small but strong community of people who understand what it’s like to live with CDA.
If you’re reading this and living with a rare condition like CDA Type 2, I want you to know that you’re not alone. Our challenges may be unique, but so is our resilience. Together, we can face whatever comes our way.
