Heart disease remains the leading cause of mortality worldwide, yet it’s largely preventable. While factors like smoking and high blood pressure are well-known culprits, another critical element often flies under the radar: apoB. This article delves into the significance of apoB, exploring its connection to heart health and providing actionable strategies to manage it.
We’ll break down the science behind cholesterol and lipoproteins, explain why apoB is a superior predictor of cardiovascular risk, and offer practical advice on lowering your levels through lifestyle modifications and, when necessary, medical interventions. Understanding and addressing your apoB levels is a proactive step towards a longer, healthier life.
This comprehensive guide covers everything from the basics of cholesterol to advanced strategies for managing apoB, empowering you to take control of your heart health. Let’s embark on this journey to understand and conquer the ‘death particle’ and pave the way for a healthier future.
Cholesterol vs. Lipoproteins
To fully understand what apoB is and its role in heart health, it’s important to first grasp the concepts of cholesterol and lipoproteins. Cholesterol, a type of fat or lipid, is essential for various bodily functions. Without it, we wouldn’t survive.
However, cholesterol doesn’t dissolve in blood, which is primarily water. To transport cholesterol throughout the body, it needs a carrier. This is where lipoproteins come into play. Lipoproteins are made of both lipids and proteins, enabling them to act as water-soluble vehicles for cholesterol transport.
These lipoproteins are classified by density, with high-density lipoproteins (HDL) and lower-density lipoproteins (LDL and VLDL) being the most commonly known. It’s a misconception to label HDL as ‘good cholesterol’ and LDL as ‘bad cholesterol.’ HDL and LDL are lipoproteins, not cholesterol itself. The cholesterol they carry is the same; the difference lies in the type of carrier.
Understanding the distinction between cholesterol and lipoproteins is crucial for appreciating the role of apoB in cardiovascular health. It sets the stage for recognizing that it’s the particles carrying cholesterol, rather than cholesterol itself, that pose the primary risk.
Understanding apoB
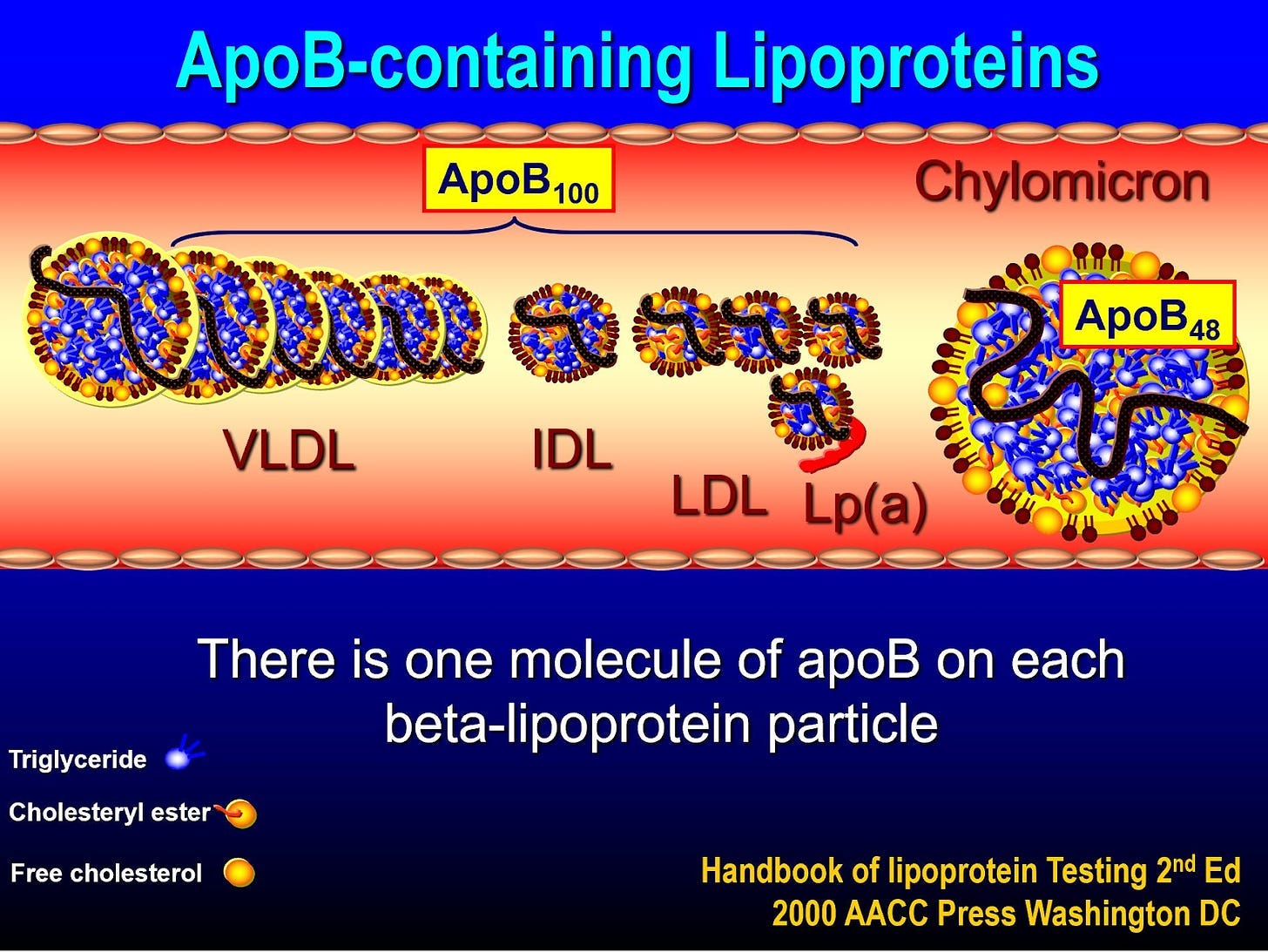
Apolipoprotein B (apoB) measures the concentration of all particles carrying this specific protein, including LDL, VLDL, IDL, and Lp(a). While many doctors use LDL concentration as a marker for Atherosclerotic Cardiovascular Disease (ASCVD) risk, apoB is increasingly recognized as a more accurate predictor.
ApoB provides a comprehensive assessment of the total number of potentially harmful particles circulating in the blood. Each of these particles can contribute to plaque buildup in the arteries, leading to heart attack or stroke.
The advantage of measuring apoB is that it captures LDL exposure in addition to other risk-driving particles like VLDL, IDL, and Lp(a). By focusing on the number of these particles, apoB offers a more complete picture of cardiovascular risk.
Therefore, understanding apoB and its relationship to ASCVD is essential for proactive heart health management. It’s not just about cholesterol numbers; it’s about the quantity of particles that can deposit cholesterol in artery walls.
ASCVD Risk Factors
Atherosclerotic Cardiovascular Disease (ASCVD) encompasses a range of conditions caused by plaque accumulation in artery walls, leading to heart attack, stroke, and other severe outcomes. Several modifiable risk factors contribute to ASCVD, including smoking, hypertension, and elevated apoB levels.
Smoking damages blood vessels and promotes plaque formation. Hypertension, or high blood pressure, strains artery walls and accelerates plaque buildup. Elevated apoB indicates a higher concentration of cholesterol-carrying particles in the blood, increasing the likelihood of plaque deposition.
While smoking cessation and blood pressure management are critical, maintaining low apoB levels is equally vital for preventing ASCVD. These three factors represent the most impactful targets for reducing cardiovascular risk.
By addressing these modifiable risk factors, individuals can significantly reduce their chances of developing ASCVD and improve their overall heart health. A proactive approach, focusing on smoking cessation, blood pressure control, and apoB management, is key to long-term cardiovascular well-being.
What apoB Should I Target?
Determining the optimal apoB level can vary depending on the healthcare professional you consult. However, a consistent recommendation is to aim for an apoB level of 50 mg/dL or below. Achieving this target often requires a combination of nutritional adjustments and pharmacological interventions.
Dr. Peter Attia suggests an even more aggressive target, recommending apoB levels between 20 and 30 mg/dL (or 30 to 40 mg/dL in some discussions), with 60 mg/dL considered the absolute maximum. Dr. Thomas Dayspring, a leading expert in lipid health, also advocates for an apoB level below 50 mg/dL.
These experts emphasize that lower apoB levels are associated with a reduced risk of ASCVD. The specific target may depend on individual risk factors and health goals, but the general consensus is that lower is better.
Ultimately, the goal is to minimize the number of apoB-containing particles circulating in the blood, reducing the likelihood of plaque buildup and cardiovascular events. Consulting with a healthcare provider to determine the most appropriate apoB target for your specific situation is essential.
Strategies to Lower apoB
Lowering apoB levels can be achieved through a combination of nutrition and, when necessary, drug interventions. While drugs often have a more significant impact, nutrition plays a crucial role in managing apoB and overall heart health.
Exercise, while beneficial for overall health, has a less direct impact on lowering apoB through lipoproteins. However, it substantially reduces ASCVD risk by improving blood pressure, metabolic health, and other factors.
Nutritional strategies primarily focus on reducing carbohydrate and saturated fat intake. A diet very low in both can effectively lower apoB but may be restrictive and difficult to maintain long-term.
The following section will delve into specific nutritional recommendations, as well as discuss various lipid-lowering medications that can help individuals achieve their target apoB levels.
Nutrition for apoB Management
Dietary modifications can significantly impact apoB levels. Key strategies include reducing carbohydrate intake to lower triglycerides and minimizing saturated fat to reduce cholesterol synthesis and improve LDL receptor function.
Lowering carbohydrate consumption reduces triglycerides, which in turn can lower apoB. Cutting saturated fats reduces cholesterol synthesis and increases the liver’s ability to remove LDL from circulation, decreasing the number of apoB-bearing LDL particles.
Consuming adequate fiber is also beneficial. Aim for 45-50g of fiber per day for males and 35-40g for females. Additionally, consider experimenting with a Mediterranean diet, which emphasizes monounsaturated fats, whole grains, vegetables, and fatty fish.
It’s essential to manage overall calorie intake, maintaining a healthy body weight, and minimizing processed foods. Remember to measure and track biomarkers to assess the impact of your diet on apoB, LDL, and Lp(a).
Lipid-Lowering Medications
When lifestyle modifications aren’t sufficient, lipid-lowering medications can play a crucial role in reducing apoB levels. Statins are typically the first-line treatment, with rosuvastatin (CRESTOR) being a common starting point.
Other options include bempedoic acid (NEXLETOL) for those who can’t tolerate statins, ezetimibe (Zetia) to block cholesterol absorption, and PCSK9 inhibitors to improve the liver’s ability to clear apoB. Fibrates can lower triglycerides, and ethyl eicosapentaenoic acid (VASCEPA) can reduce LDL in patients with elevated triglycerides.
Peter Attia’s personal protocol involves a PCSK9 inhibitor, NEXLIZET (bempedoic acid and ezetimibe), and a statin. Consulting with your doctor to determine the most appropriate medication regimen is essential.
Statins, despite potential side effects like muscle aches and liver function elevations, are generally considered safe and effective. Regular monitoring and open communication with your healthcare provider are crucial for managing any potential adverse effects.
Next Steps and Conclusion
Start by requesting a comprehensive lipid panel from your doctor, including apoB and Lp(a). Ask for a liver function test to establish a baseline if you consider statins.
Be proactive, patient, and persistent in advocating for your heart health. Many doctors focus on treating existing disease rather than preventing it, so be prepared to educate yourself and advocate for your needs.
Explore resources like Peter Attia’s podcasts and Thomas Dayspring’s social media for additional information. By combining proactive lifestyle changes with appropriate medical interventions, you can significantly reduce or eliminate your risk of ASCVD.
In conclusion, understanding and managing apoB is a critical step in preventing heart disease. By adopting a comprehensive approach that encompasses nutrition, exercise, and, when necessary, medication, you can take control of your cardiovascular health and pave the way for a longer, healthier life.