People often ask me if I miss clinical care. I spent 10 years working in outpatient physical therapy before transitioning to a health tech startup. I never hesitate with the answer.
I don’t.
I’m not alone in that feeling. Healthcare providers are leaving clinical care and there aren’t enough incoming replacements to meet the needs of Americans. It’s not restricted to physical therapy.
There is about 1 doctor for every 310 Americans and the trend is moving in the wrong direction. Physicians are aging and more are approaching retirement than are joining the workforce. Almost half of all physicians are over 55. More are transitioning out of clinical care mid-career than in the past.
The current trends will leave massive provider shortages across the US. This will lead to longer wait times and subsequent delays in care. Preventative care will be less common and health outcomes will suffer. To fill the gaps, people will have to pay extra for healthcare access, such as concierge care.
There isn’t a single cause or fix to the workforce shortage, but there are two large drivers that need to be addressed. The first has a direct impact on the appeal of a healthcare career.
The cost of school is too high
Every time student loan forgiveness is brought up the “pay back what you borrowed” crowd shows up. I agree, that debts should be paid. There is a large ‘but’ concerning student loans.
The system is broken.
The loans offered to 18–22-year-olds without other means to pay for schooling (family money and scholarships cover a small proportion, far below the number of providers our country needs), are predatory. They are high interest (approaching 7%) and interest accrues as soon as they are taken out. Payments are on hold until 6 months post-graduation, but the total bill keeps rising.
How many people do you know that have over $300,000 dollars readily available to pay for 8 years of schooling (undergrad plus grad)?
The average cost of medical school is $167,476 for in-state, public schools and$275,068 for out-of-state or private schools. That just accounts for tuition, fees, and health insurance. The cost of living adds significantly more costs. Don’t forget about the $10,000-30,000 annual tuition costs for undergrad.
Gone are the days when you can pay your way through school. Tuition growth has far exceeded wage growth. Over the past 25 years, college costs have increased by 188% compared to a meager 26% for wages.
This leads to astronomical student debt.
In 2024, 28,000 students graduated from US medical school. They left with an average student loan debt of $243,483. With the high interest rates, it takes most doctors 10–30 years to pay off the medical loan debt alone. Taking on undergrad debt pushes the number closer to 30 for most.
The situation is just as bad for other providers when you account for their income and ability to pay off their debt. Take nurses as an example.
The average student loan debt for nurses is close to $20,000 for an associate’s degree, $50,000 for a master’s degree, and $190,000 for a doctorate (nurse practitioners). For physical therapists with a doctorate (the standard degree for the past 20 years), student loan debt is close to $150,000.
Not exactly an enticing selling point for students considering which career to pursue.
The debt has major lifestyle implications. Doctors and nurses are pushing back buying a house, buying a car, and going on vacation.
So, while doctors can make good money, the debt burden wipes out the income. Physical therapists and nurses are hit even harder, as they don’t have the same income ceilings.
And cost of schooling is only one of the major issues fueling a workforce shortage. There is another major issue that is impacting the appeal of a job in healthcare and thus the pipeline. It also impacts the likelihood someone stays in clinical care.
It is the reason I left.
Private insurance is killing healthcare
How long do you think it takes for a provider to document a patient visit?
I taught for a physical therapy residency program for 7 years. My goal for my residents was to get their evaluation notes under 20 minutes, progress notes under 10, and daily notes under 5 minutes by the end of their first 90 days. Those goals eventually reached 10, 5, and 2 minutes.
Now add up a day consisting of 2 evaluations, 2 progress notes, and 8 daily notes. Even a highly efficient clinician is documenting for close to an hour in a full day. Often, these notes are completed during lunch (unless other meetings take place) or after work hours.
Then, layer in insurance authorizations, discharge summaries, plan of care updates, and home exercise program designs. The administrative burden adds up.
Making matters worse, all of those numbers are increasing every year.
Insurance companies layer on additional administrative burdens every year. Prior authorization has become more common and more rigorous. Visit caps are shortened, requiring more authorization requests. Documentation requirements to justify care are expanded.
All this happens without increasing reimbursement.
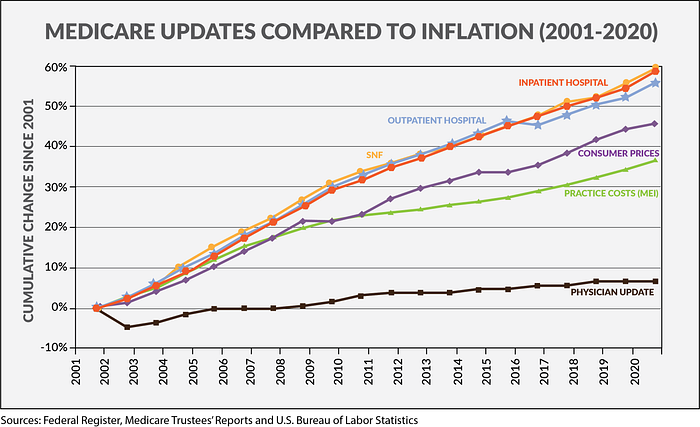
You can see in the graph above that Medicare is not keeping up with the costs of care.
Student loans are going up.
The cost of living is going up.
Medical costs are going up.
But reimbursement is decreasing.
So, if expenses are rising but revenue per encounter isn’t, how do hospitals and practices keep up with salary demands? Clinicians expect to make more as their loans and the cost of living go up. There is only one way to make the math work.
Higher productivity.
And this drives more burnout and masses of clinicians to leave patient care. Providers want to help people. It’s why most of us got into the profession. But the administrative burden is crippling.
The status quo is not sustainable.
Are there any solutions?
The growing shortage of healthcare providers stems from multiple factors. I have focused on what I believe are the three primary drivers: student debt, administrative burdens, and low reimbursement rates. While the problem is complex, there are several key solutions that could help reverse these trends and improve provider supply.
1. Reducing the Financial Burden on Medical Students
High school debt discourages many potential providers from entering the field, particularly in lower-paying primary care roles. Expanding loan forgiveness programs and increasing funding for scholarships targeted at primary care and rural medicine could help make these career paths more attractive. Addressing the costs of medical education — through tuition reform or government investment in training programs — could lower financial barriers to entry.
2. Easing Administrative Burdens
Reduce the $83 billion spent annually on administrative overhead. Some strategies include streamlining documentation. I can attest to the many unnecessary requirements. Improving electronic health records (EHR) usability and reforming insurance policies would allow providers to spend more time with patients and limit documentation time.
3. Adjusting Reimbursement Models and Reforming Insurance Practices
Medicaid and some private health insurance plan reimbursement rates often fail to cover the full cost of care, putting financial strain on providers and health systems. Physicians recently faced another round of pay cuts under Medicare. Policymakers must consider adjusting reimbursement rates to ensure fair compensation for providers, especially in primary care and critical specialties. Without competitive pay, provider shortages will only worsen.
In the private sector, health insurers wield significant power over providers, with large companies dictating payment structures and prior authorization processes that delay care. A lot of providers have reached their breaking point. Every week, I see another physical therapy practice dropping United Health Care, deciding out-of-network is more financially viable.
Policymakers should introduce regulations that prevent excessive insurance roadblocks, enforce timely reimbursements, and ensure that coverage decisions prioritize patient care over profits. Addressing inefficiencies in Medicare Advantage, particularly around questionable risk adjustments and denials of necessary care, is also critical.
4. Expanding the Workforce Beyond Physicians
While increasing the number of doctors is essential, expanding the roles of nurse practitioners, physician assistants, physical therapists, and other healthcare professionals can help address gaps in care.
The average wait time has risen to 26 days. Seeking a physical therapist at the beginning of a plan of care can reduce wait times and save the healthcare system substantial money, preventing unnecessary services.
5. Leveraging Technology Wisely
Artificial intelligence (AI), automation, telehealth, and remote patient monitoring can enhance efficiency, but they cannot replace the need for more providers. Instead of viewing technology as a cure-all, health systems should focus on using it to support providers — reducing their workload, improving diagnostic accuracy, and optimizing patient scheduling to minimize bottlenecks.
AI can facilitate a hybrid model, which can expand patient access, reduce administrative burden, and improve outcomes.
Moving Forward
Addressing the healthcare provider shortage requires a multi-pronged approach. Financial relief for medical students, reduced administrative burdens, better reimbursement models, and expanded workforce strategies can help stabilize provider supply. Without meaningful action, provider shortages will continue to worsen, further straining an already overburdened system.
While I left clinical care, I did not leave healthcare. The startup I joined helps practices expand their direct pay options. It heavily focuses on direct-to-employer models of care. This model aligns self-insured employers with providers to provide the best outcomes for patients and a fair reimbursement rate.
The only losers in the model are private insurers.
Now is the time for policymakers, healthcare leaders, and industry stakeholders to work toward sustainable solutions that prioritize access, affordability, and fairness in care delivery.
